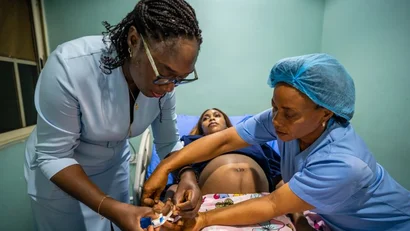
Millions of children have never had a single vaccine. Finding them isn’t enough

The world has gotten good at identifying unvaccinated children. The harder problem is making sure we can reliably reach them.
Every year, millions of children grow up with no protection against diseases that vaccines have made preventable. In 2024, an estimated 14.3 million children were zero-dose, meaning they had never received a single vaccine. No first jab. No record in routine health system. Millions more start but do not complete the routine immunization schedule. More than half of the world’s zero-dose children are concentrated in a small number of countries, including Ethiopia, the Democratic Republic of Congo, India, Indonesia, Nigeria, and Pakistan. Many live in remote, rural, or conflict affected areas, or are displaced, highly mobile, and living in communities that health systems struggle to consistently reach. Rapid urbanization is compounding the challenge: by 2050, nearly 68 percent of the global population is projected to live in cities, and a growing proportion of zero-dose children live in rapidly expanding informal urban settlements where traditional approaches struggle to reach them. The challenge is not just geography. It is how health systems are designed.
The global health community has gotten good at identifying who is missed and why. But the harder problem is how to ensure those children complete their vaccine schedules. The response often takes the form of new initiatives, campaigns, or vertical programs—sitting alongside routine systems rather than changing them. The only sustainable path, financially and operationally, is to fold zero-dose efforts to reach and retain children into how routine immunization systems work every day. The barriers keeping children unreached differ by context and shift over time, so what that integration looks like will also differ from one place to the next.
Why children are missed
Three barriers shape whether children get vaccinated: access, intent, and health system readiness. Their relative importance varies by context and shifts over time—which is why the response and mix of interventions must adapt accordingly.
Access barriers look different depending on where you are. In some areas, distance and mobility are the primary constraints. In others, it is whether a clinic is open at a time a working caregiver can attend, or whether services are available at all. Intent is about more than awareness. Caregivers do not just need to be convinced to vaccinate their children; they need services they can rely on. When previous visits ended in stock-outs or cancelled sessions, caregivers stop coming back. Health system readiness is often the most decisive factor. Even when countries know where zero-dose children live, they may struggle to reach them if vaccines are unavailable, last-mile cold chain logistics are unreliable, or outreach lacks consistent funding.
Integration in practice
Cambodia, Ethiopia, and Indonesia show what it looks like to respond to these barriers and embed that response into routine systems across very different contexts.
In Cambodia, access, particularly timing of services rather than distance, was often the dominant barrier in urban and border areas. Services ran at times when working families and migrant populations couldn't attend. To address this, border outreach was deployed at Thai-Cambodia crossing points during major holidays, targeting migrant workers across four districts. Clinic hours were extended across more than forty health centers in seven districts to reach urban workers who couldn’t attend during standard hours. These were not parallel campaigns. Existing health center staff ran the outreach. Extended sessions were integrated with nutrition and de-worming services. As a result, in just one year, the share of zero-dose children reached nearly doubled.
In Ethiopia, health system readiness at the primary care level was often the binding constraint across diverse settings. Strengthening planning, mentoring, and tracking of children under two—the age at which most routine vaccines should be given—helped translate zero-dose identification into more consistent outreach and follow up. In urban Addis Ababa, vaccination sessions were integrated with nutrition, deworming, and other services, reducing the time and loss of income that kept working caregivers away. In nomadic communities in Afar, service delivery was adapted through engagement with trusted local leaders, who helped identify and link mobile populations to services. In Oromia’s farming communities, community dialogue with traditional healers addressed cultural barriers that formal health messaging had failed to shift.
In Indonesia, the challenge was health system readiness; specifically, data to accurately identify who truly hadn't been vaccinated. Gaps in reporting from private facilities meant some vaccinations weren't captured in national tracking, creating false zero-dose cases. Integrating private sector vaccination data into the national registry and combining it with geospatial mapping —helping health facilities better understand their catchment areas and plan where to place immunization posts — gave health authorities a more accurate picture of where to focus. More than 220,000 false zero-dose records were corrected, and coverage among truly unreached children increased by up to 6 percent.



Image 1: Free cervical cancer vaccination program for schools in Cambodia (Copyright: CHAI). Image 2: Pneumococcal conjugate vaccine (PCV) training in Bogor, West Java, Indonesia (Copyright: Yanti Leosari/CHAI). Image 3: Vaccines department at North Gondar Health in Ethiopia (Copyright: CHAI).
Sustainable by design
Vaccination remains one of the most cost-effective public health interventions available. As donor funding plateaus and domestic co-financing obligations grow, evidence of what works must be paired with evidence of what works at sustainable cost. Governments face hard choices: which interventions to fund, where to deploy them and how to sequence them, and what trade-offs to accept when operating under constrained budgets.
Operational reliability is central to this. Estimates suggest up to 50 percent of vaccines may be wasted globally, due to cold chain and logistics challenges. When clinics cancel sessions because the vaccines didn’t arrive in time, it erodes community trust and drives dropout rates. Reliable supply chains are not just a technical requirement. They are what keeps caregivers coming back for every dose their child needs.
But service delivery reliability is shaped upstream — by market dynamics and purchasing decisions. The introduction of products like HPV, malaria, and maternal vaccinations is increasing program complexity. Product characteristics drive cold chain requirements. Pricing determines what governments can afford to sustain. Supply predictability underpins effective planning. When these decisions are not aligned with delivery realities, new vaccines risk overwhelming the very systems meant to deliver them.
Every child, every system
With more than fourteen million zero-dose children globally, the challenge remains substantial. Progress depends on moving beyond identification toward strengthening the systems that deliver vaccines every day.
Rather than adding parallel programs, organizations that work across delivery and market shaping can help governments embed this approach into how their systems already work. The Clinton Health Access Initiative (CHAI) works with ministries of health in over twenty African and Asian countries to strengthen immunization programs. CHAI’s experience across Cambodia, Ethiopia, Indonesia, and beyond shows the approach is replicable even when the specific intervention is not: diagnose the dominant constraints; adapt the routine system; integrate rather than create parallel tracks.
To learn more about CHAI’s approach to immunization systems strengthening, contact Alexio Mangwiro, Senior Director, Vaccines at CHAI [amangwiro(at)clintonhealthaccess.org].
We invited Alexio Mangwiro, Senior Director, Vaccines at CHAI, to share his insights on what it takes operationally to reach zero-dose children and to close the immunisation gap, as the world marks World Immunization Week from 24-30 April. The views expressed are his own and do not necessarily reflect those of the Global Health Hub Germany.
Related Articles
![[Translate to English:] [Translate to English:]](/fileadmin/_processed_/d/b/csm_Design_ohne_Titel__6__894bf9a994.webp)