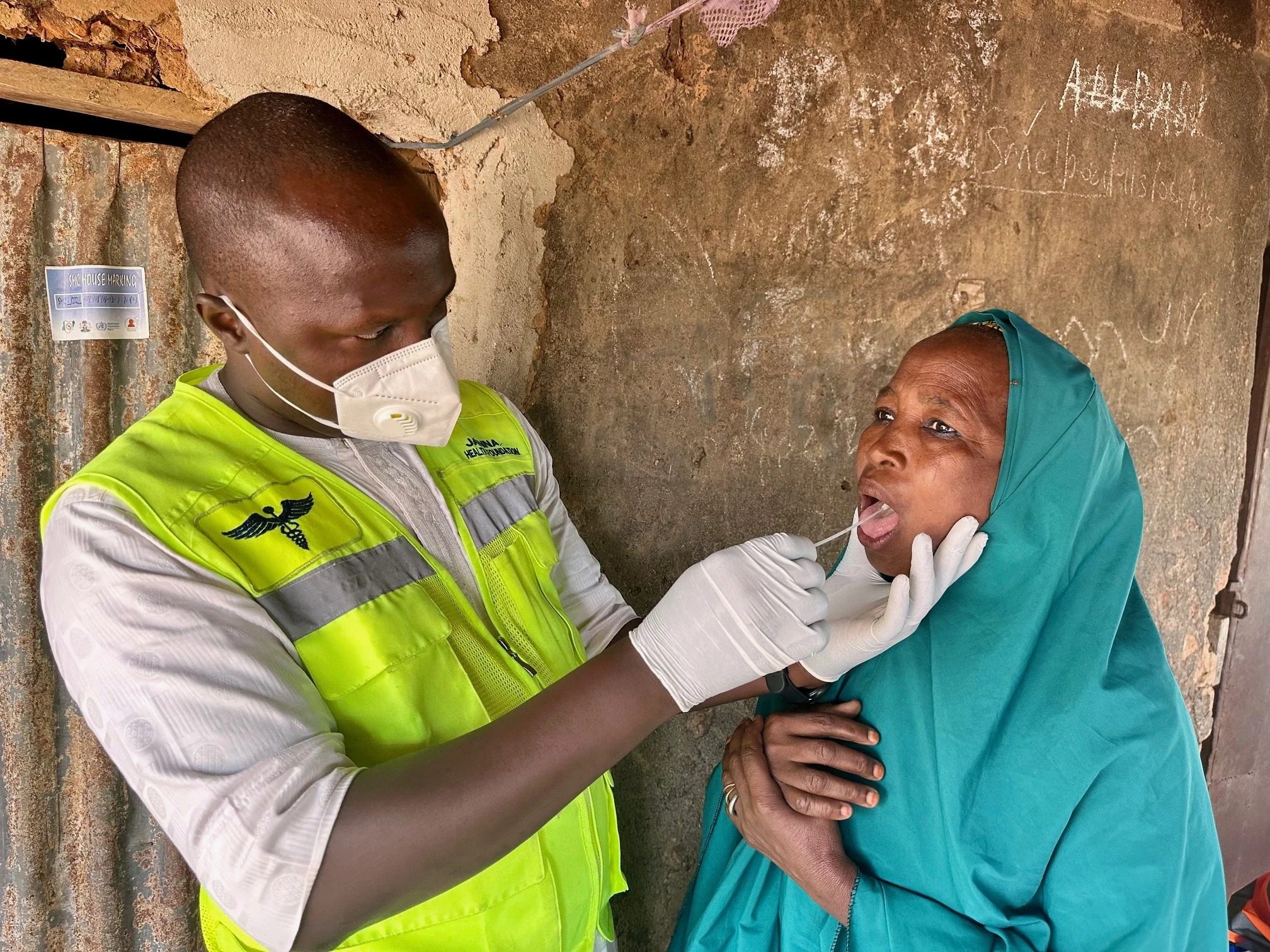
Do the Ingredients for Ending TB – Country Ownership and Global Solidarity – Exist Today?

Tuberculosis (TB) is preventable and curable, yet still kills millions. Are country ownership and global solidarity strong enough today to finally end TB?
TB is everyone’s problem. Like all airborne diseases, TB does not respect borders. Without strong national ownership, sustained political commitment, and genuine global solidarity, it will remain the world’s leading infectious disease killer, as it was before COVID-19 and once again is today. We are living through challenging and uncertain times. The social, economic, and political landscape is shifting rapidly, often faster than governments and leaders can interpret or respond. Global health ambitions are fading, and targets once considered achievable are drifting out of reach.
However, TB does not allow for retreat. Every undiagnosed and untreated person fuels transmission, creating a compounding effect where each missed case leads to many more. It is a silent and relentless snowball, growing with every delay in diagnosis and treatment. The situation is even more alarming with drug-resistant TB (DR-TB), where progress in diagnosis and treatment has stagnated for over a decade, leaving countries struggling to contain it and becoming a threat to health security and public health.
For years, national TB responses have been driven by dedicated professionals working quietly and often invisibly. Despite being undervalued, underfunded, and sometimes stigmatized, they have sustained fragile systems and delivered services under difficult conditions.
Two major disruptions are reshaping this dynamic. The COVID-19 pandemic brought renewed attention to airborne diseases and highlighted the expertise within TB programmes. At the same time, changes in the global financing landscape since 2025 have forced governments to confront difficult questions: which diseases most affect their populations, and how can they be addressed with national resources?
This moment of reckoning, strengthened by years of advocacy from the Stop TB Partnership and its partners, has pushed TB back into national focus, despite the challenges. Governments are increasingly looking inward, assessing their data, systems, and responsibilities. This creates an opportunity, but also a test of leadership.
Country Ownership Is Essential to End TB
Country ownership is not a declaration; it is a must and a practice. It requires discipline, clarity, and long-term commitment, grounded in evidence.
First, it requires knowing the data. Reliable, high-quality national data systems are essential. Countries must be able to collect, analyse, and use their own data to understand the scale and nature of their epidemic and diseases. Parallel systems created by external partners may provide temporary support, but they cannot replace strong national systems that are sustainable and fully owned.
Second, it requires understanding the response. Governments need a clear picture of what is working and what is not. This includes ensuring that plans are realistic and responsive to on the ground realities.
Third, sustainable financing is critical. Multi-year budgets must be developed based on actual needs, not assumptions. TB responses cannot depend solely on short-term funding cycles. They require predictable and sustained investment that allows for planning, scaling, and maintaining services over time.
Fourth, prioritization is essential. Resources are limited, and countries must make strategic choices about how to allocate them. This means balancing domestic funding with support from bilateral and multilateral partners, while also exploring innovative financing mechanisms. It also requires investment in innovations - adopting new tools for diagnosis that bring it closer to where people live and accessible to everyone as well as innovations that allow for multi-disease screening and diagnosis.
Country ownership means that TB is no longer treated as a peripheral or vertical issue, but as a central component of national health, economic stability, and social development.
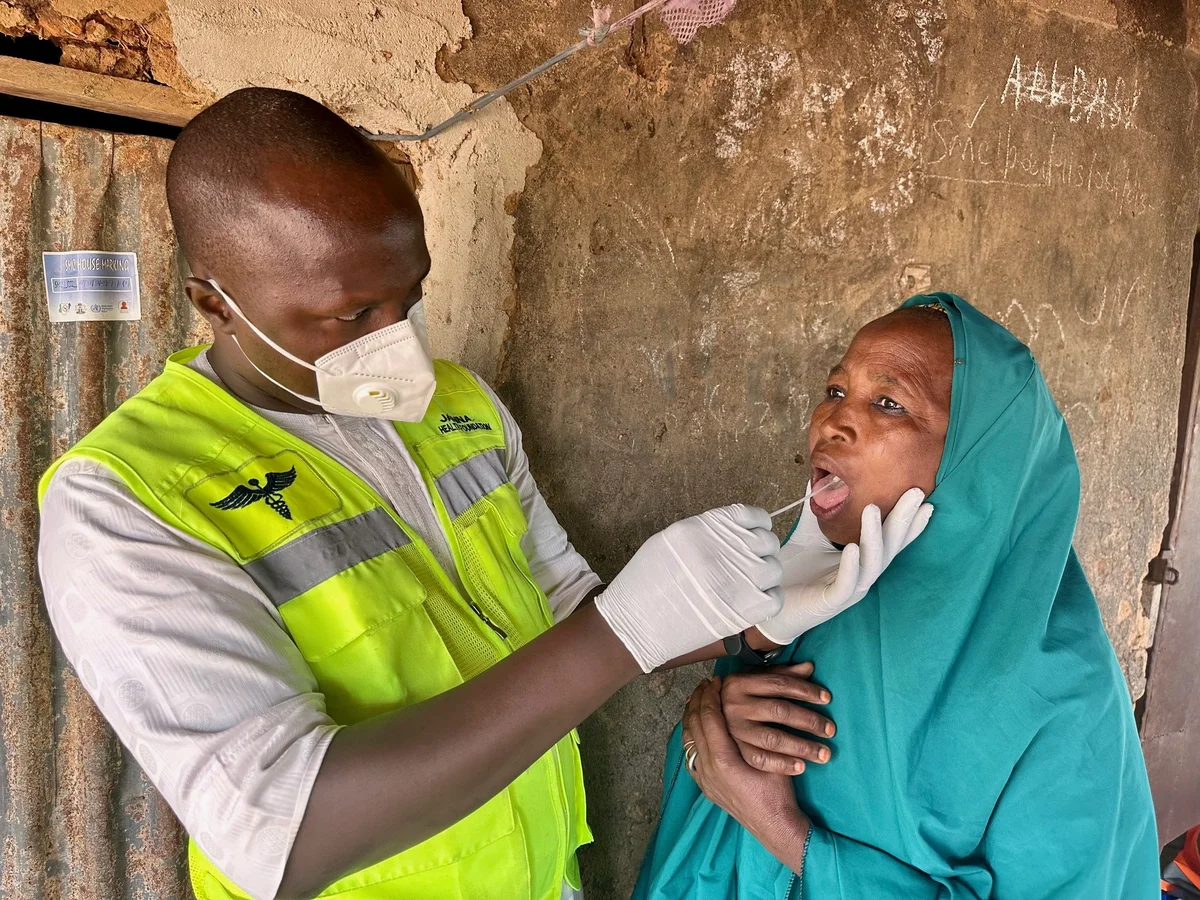
The Indispensable Role of Global Solidarity
Country ownership alone is not enough. TB knows no borders and, as long as we have TB everywhere in the world and as long as we breathe – we are all at risk.
TB thrives in conditions of poverty, undernutrition, overcrowding, and limited access to healthcare. These are not challenges that any one country can solve in isolation. Global solidarity is therefore not optional; it is essential.
Research, data sharing, and coordinated responses are essential to address emerging challenges, including drug resistance and the intersection of TB with other health and social issues. Without global collaboration and solidarity this will not happen. New diagnostics, medicines, and vaccines must be made available to all countries, not only those that can afford them first. Delayed access prolongs the epidemic and moves the target to End TB further away.
It means sustained international financing. While countries will need to eventually cover the costs of their own TB response, many high-burden countries are not there yet and while they scale up their investments, predictable external support remains critical, particularly for early diagnosis and access to diagnosis and care for everyone, introducing new technologies, and addressing drug-resistant TB.
In the context of TB, global solidarity also means maintaining the markets for medicines, diagnostics and other essential commodities. It means working together and aligning efforts to reduce the price of commodities and ensure everyone has access to them.
Global solidarity requires shared accountability. Commitments made must translate into real action. Countries, donors, global institutions, communities and civil society all have roles to play, all are accountable and progress must be measured transparently.
At a time when geopolitical tensions are increasing and multilateral cooperation is under pressure, global solidarity is being tested. Yet TB offers a clear and urgent reminder: infectious diseases do not recognize borders, and fragmented responses will always fall short.
Do These Ingredients Still Exist?
The answer is both encouraging and concerning.
There are clear signs that country ownership is strengthening, driven by necessity, a growing recognition of TB’s impact on national health and economies, and the leadership of some of the highest TB-burden countries, which are serving as examples to the world.
At the same time, global solidarity shows signs of strain. Competing priorities, economic pressures, and shifting political landscapes reduce the level of international cooperation and support that has been critical in in the global health arena in the last years.
So, both ingredients exist, but they are fragile and need to be supported.
Without deliberate and sustained effort, they risk being weakened at precisely the moment when they are most needed. Ending TB is not a question of whether we have the tools or knowledge. It is a question of whether we have the collective will.
Will countries fully own their responses and invest in their people and for their people with TB? Will the global community act in solidarity and uphold its commitments, or walk away and roll back hard-won progress?
If both answers are yes, ending TB is within reach. If not, TB will continue to persist, not because it cannot be stopped, but because we choose not to stop it.
We invited Dr. Lucica Ditiu, Executive Director of the Stop TB Partnership, to share her insights on sustaining the fight against tuberculosis in a changing global health landscape, as the world marks World TB Day on 24 March. The views expressed are her own and do not necessarily reflect those of the Global Health Hub Germany.