The art of policymaking: lessons from the 2026 Health Policy Trend Report

At the Berlin University Alliance Grand Challenges Conference in March 2026, the Health Policy Trend Report 2026 was launched, mapping the evolving challenges, opportunities, and solutions in health policymaking.
Sascha van Beek, Member of the German Parliament and UNITE, opened the launch with a keynote, followed by a cross-sector discussion between Tatjana Gust of the Bayer Foundation and Philip AbdelMalik of the WHO Hub for Pandemic and Epidemic Intelligence.
The report was developed by the Global Health Policy Lab (GHPL), in partnership with the African Population Health and Research Center (APHRC) and UNITE Parliamentarians Network for Global Health (UNITE).

A global survey, and the obstacles that keep appearing
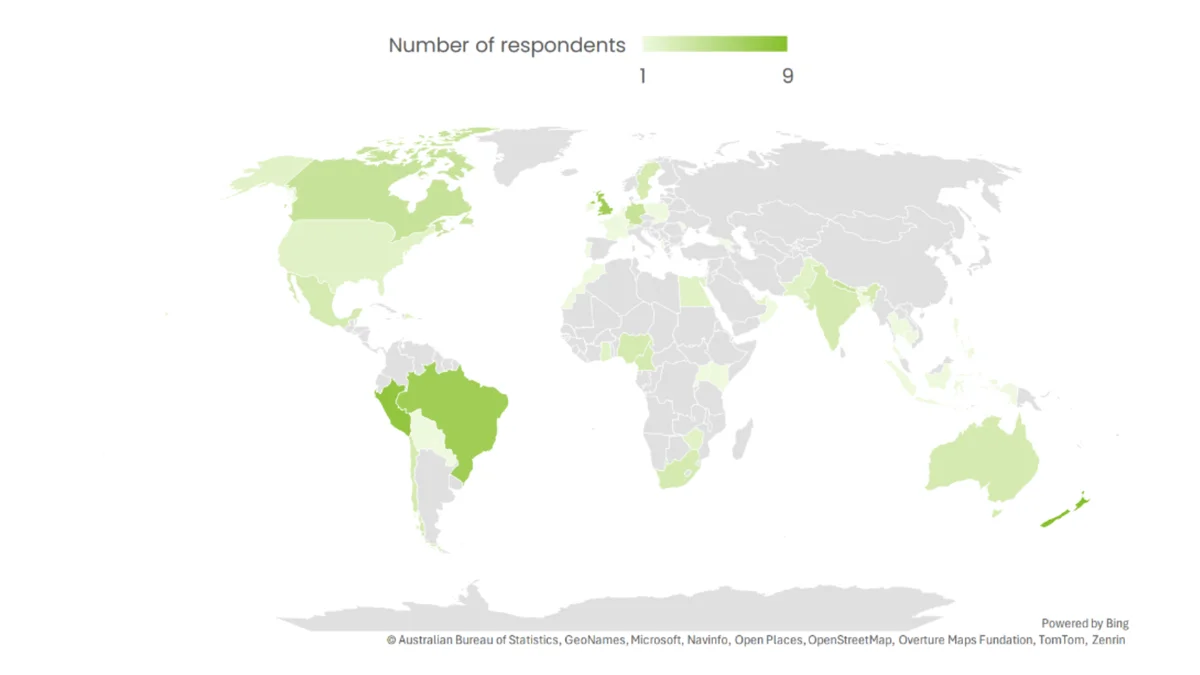
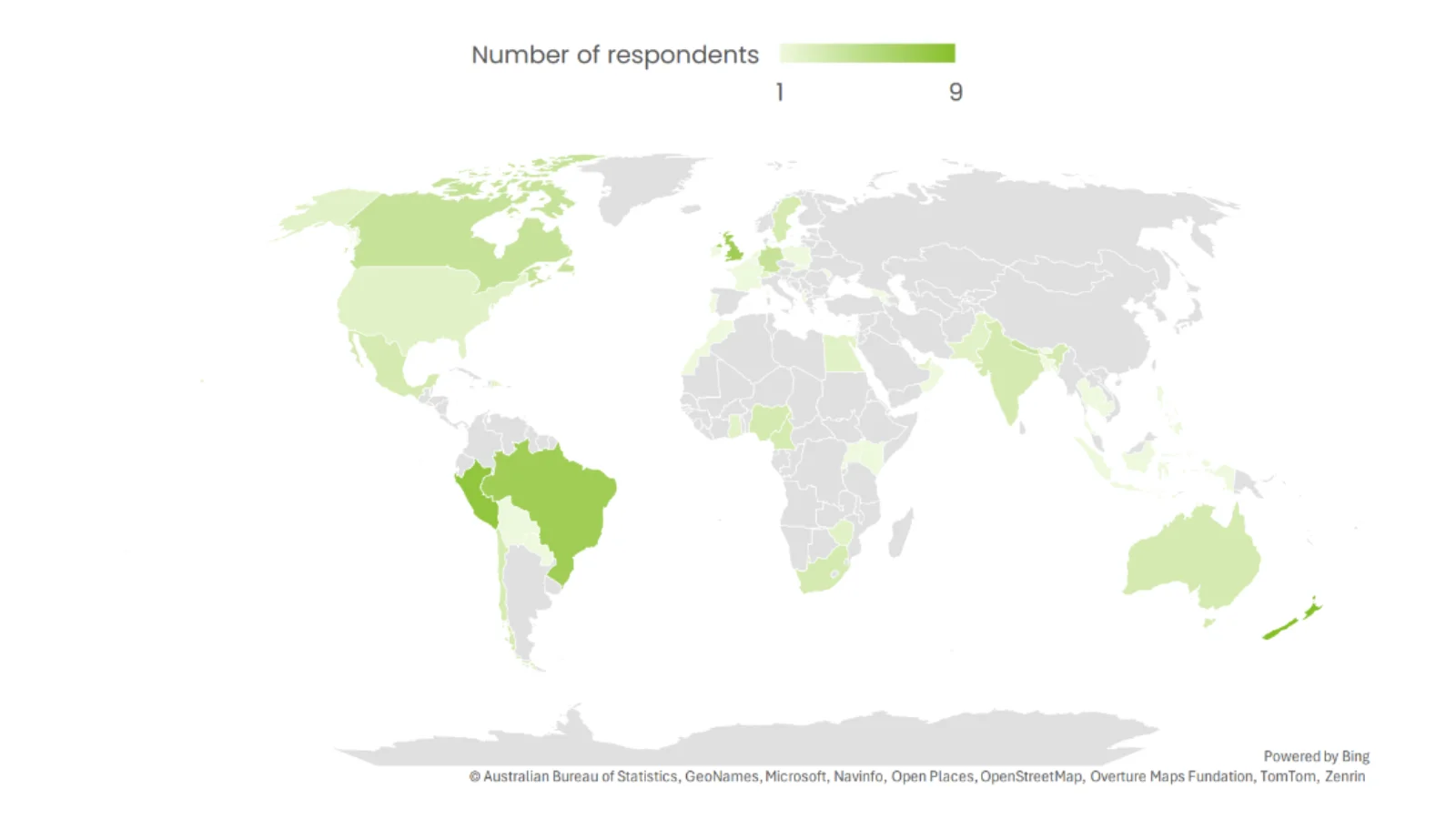
Figure 1: Geographic distribution of survey respondents across 49 countries (n=109). Source: Nature Research Intelligence (2025), commissioned by the Global Health Policy Lab.
The empirical backbone of the Health Policy Trend Report is a survey of 109 policymakers across 49 countries, spanning all five continents, conducted in collaboration with Nature Research Intelligence. The survey findings are striking less for their novelty than for their consistency. Across contexts, the same constraints surface again and again.
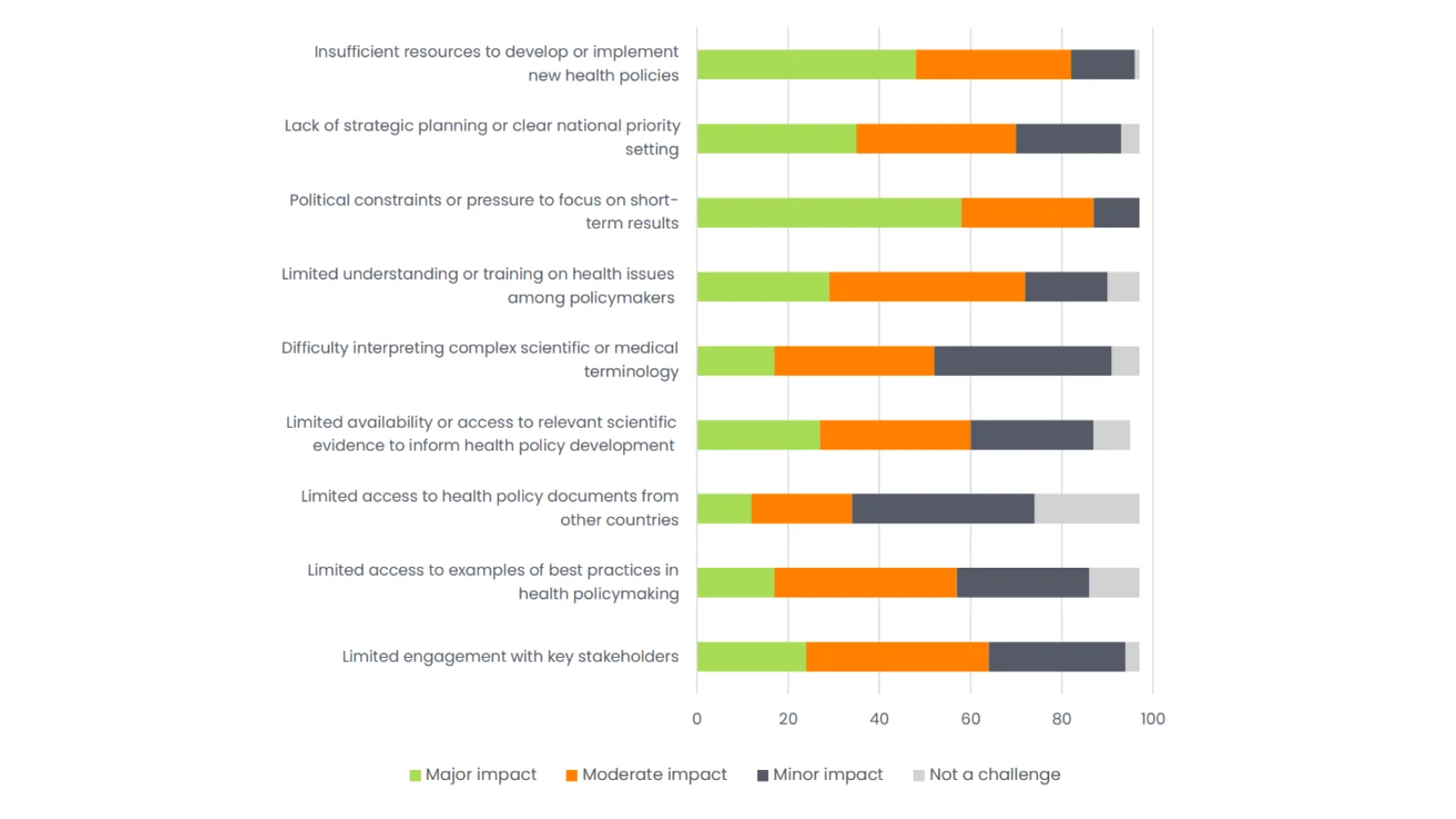
- Short-Termism: Ninety percent of respondents cited the pressure of electoral cycles as a major challenge. Political incentives favour ‘ribbon-cutting’ over long-term prevention; cabinet reshuffles often kill reforms before they can mature.
- Resource and Information Scarcity: Beyond tight budgets, 44% of surveyed policymakers struggle to find or compare international best practices. Relevant evidence remains buried in institutional silos or locked behind language barriers, leading to a ‘chronic reinvention of wheels’.
- The Expertise Gap: Nearly three-quarters of respondents acknowledged limited health literacy. When policymakers cannot confidently interpret technical data, they risk ‘policy capture’ by external advisers who may not be transparently integrated into the decision-making process.
Together, these obstacles, among others, carry a measurable cost. The report cites a figure that should discomfort anyone working at the intersection of research and policy: on average, it takes 17 years for scientific evidence to translate into routine practice. At the WHO's 2023 Global Evidence-to-Policy Summit, leaders noted that only about 14 percent of research ultimately reaches policy or practice at all.
APHRC's Catalyze Impact Initiative, applied in Ethiopia and Nigeria, offers a counterpoint. By embedding iterative feedback loops directly into the policymaking cycle, including co-designing research agendas with local stakeholders, testing interventions rapidly, and adapting based on results, the initiative reduced the lag between evidence generation and policy uptake to four years or less. In Lagos, a sample registration system was established to generate timely data on maternal deaths occurring outside health facilities. This produced information that had simply not existed before, and without which no timely policy response was possible. Ethiopia developed a National Research Roadmap through inclusive stakeholder consultations that translated evidence synthesis into an actionable national strategy.
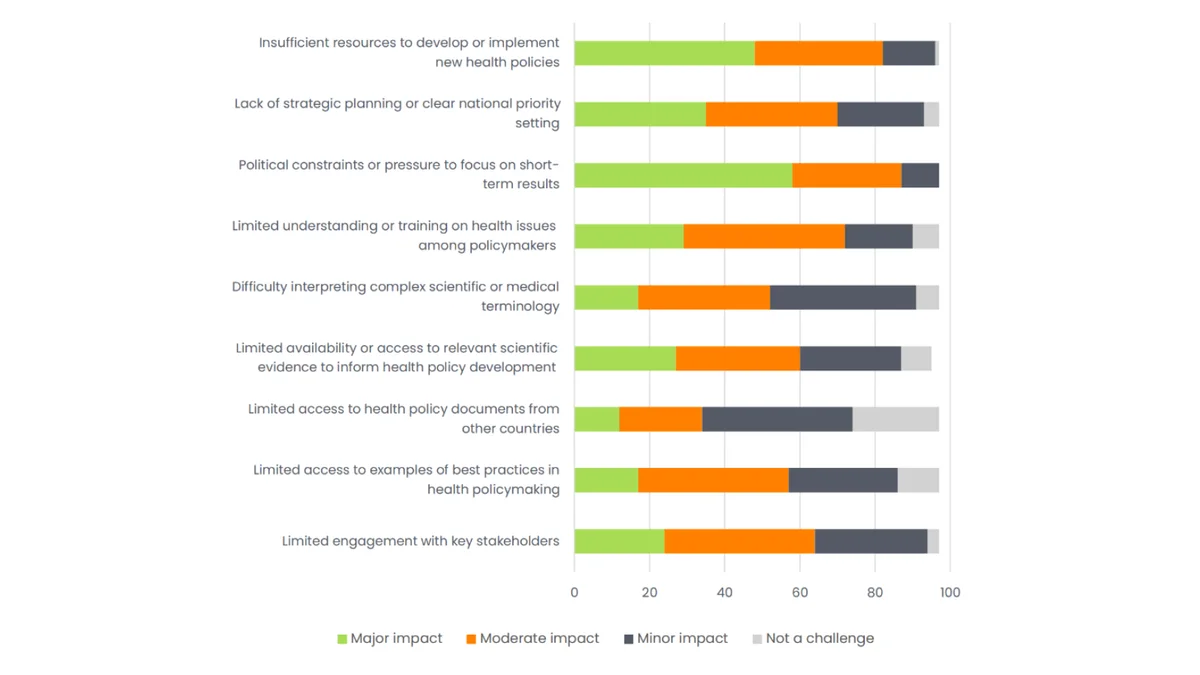
Figure 2: Extent of the challenges to health policymaking experienced by respondents (n=97). Source: Nature Research Intelligence (2025), commissioned by the Global Health Policy Lab.
What actually works
The more instructive part of the report is its case studies, drawn from seven countries: Egypt, Ireland, Mexico, Australia, the United Kingdom, Canada, and Germany. Contributed by former and sitting parliamentarians, they demonstrate that the barriers in health policymaking are real but not insurmountable, and that effective responses tend to share certain features.
In Ireland, a hung parliament forced fourteen legislators from across the political spectrum to develop a shared health reform agenda together. Supported by academic advisers from Trinity College Dublin and the European Observatory acting as ‘honest brokers’, the process produced Sláintecare, a ten-year universal healthcare plan that has survived elections, cabinet reshuffles, and a pandemic without being disowned by any major party. The durability itself was the policy outcome.
Egypt's elimination of hepatitis C, achieving WHO gold-tier status in 2023 with prevalence falling from roughly six percent to around 0.4 percent in six years, illustrates what becomes possible when political commitment is total and coordination is centralised. A whole-of-government approach, state-funded treatment, government-negotiated affordable drug pricing, and a digital platform managing over 60 million screenings combined to produce what the report estimates will yield economic gains exceeding $7 billion by 2030. The case also demonstrates that short-term political pressure, usually a constraint on reform, can be redirected: when a president makes disease elimination a national priority, the same pressure that stalls structural change can accelerate it.
A sequenced approach to change
The report’s recommendations are sequenced across three time horizons, which in itself makes a case: durable change is incremental.
The Short Term (0–2 Years): Leverage Technology
The priority is reducing ‘information asymmetry’. The report advocates for AI-assisted evidence synthesis and digital repositories, such as GHPL’s own Digital Repository for Health Policy, to help overstretched teams borrow from international peers and adapt proven approaches to local contexts.
The Medium Term (3–5 Years): Make evidence-use the default
Evidence use must become a procedural requirement. Following the model of Ghana’s National Public Policy Guidelines, all policy documents should include concise evidence briefs and monitoring frameworks. This must be paired with professional development for parliamentary staff in health literacy and digital governance.
The Long Term (5+ Years): Secure structural reform and overcome silos
The ultimate goal is the ‘Health in All Policies’ approach. By embedding health outcomes into the budgeting processes of finance, housing, and education ministries, as seen in Finland’s North Karelia Project, governments can ensure that health gains outlast the next election.
The foundation the report lays out is clear. As one survey respondent put it: ‘Borrow brilliance, adapt what works elsewhere to fit here.’ That is, in a nutshell, what the Health Policy Trend Report 2026 suggests policymaking stakeholders to do.
We invited Rebecca Ohanes, Branwen Hennig, Michael Bayerlein und Hendrik Oye from the Global Health Policy Lab, to share the key findings from the “Health Policy Trend Report 2026.” The views expressed are their own and do not necessarily reflect the positions of the Global Health Hub Germany.
Related Articles